Addiction & Chronic Pain Treatment Options in Connecticut
We will work with you to develop a wellness program for the care and treatment you need.
Connecticut Addiction Medicine, LLC. would like to be your partner in health care. Feel free to ask your questions and share your concerns with us.
Services provided include the following:
- Outpatient detoxification
- Addiction/Psychiatric evaluation
- Pain Management
- Psychosocial evaluation
- Individual counselling and psychotherapy
- Family Therapy
- Group (relapse prevention) therapy
- Addiction education
- Urine toxicology testing utilizing methods that provide the highest level of accuracy.
- Screening for associated medical problems
- Medication management
- Suboxone (buprenorphine/naloxone) therapy
- Vivitrol (injectable naltrexone) therapy
- Participation in Twelve-Step Recovery (eg. AA, NA) is encouraged
- Working relationships with the criminal justice system
Close working relationships with treatment centers
that provide a higher level of care including:
- Inpatient detoxification
- Intensive Outpatient (IOP)
- Partial Hospitalization (PHP)
- Residential (28-day,45- day and 90-day)
Eligibility Requirements:
- At least 16 years of age
- Active substance abuse disorder
- Have a photo ID and proof of insurance
- Agree to adhere to program policies and procedures
All patients are seen within 24 hours and they are treated with dignity and respect.
Pain Management
At Connecticut Addiction Medicine, in addition to treating patients with substance abuse, we provide optimal medical management of chronic pain from many origins, especially musculoskeletal. Primary treatment is with Suboxone(R), commonly used in conjunction with ancillary non-opioid medications. For patients currently on chronic opioid therapy, conversion to Suboxone(R) is readily achieved in the office within the first month. The majority of patients receive greater than 50% improvement in their chronic pain. If needed, referrals may be made to hospital-based pain management centers for interventional therapies.
Suboxone(R) has the following advantages compared to usual opioid therapy:
- No significant adverse affects
- No risk of misuse or overdose
- No development of tolerance
- Proven to be more effective than traditional chronic opioids.
Most Common Medications Used for Treatment
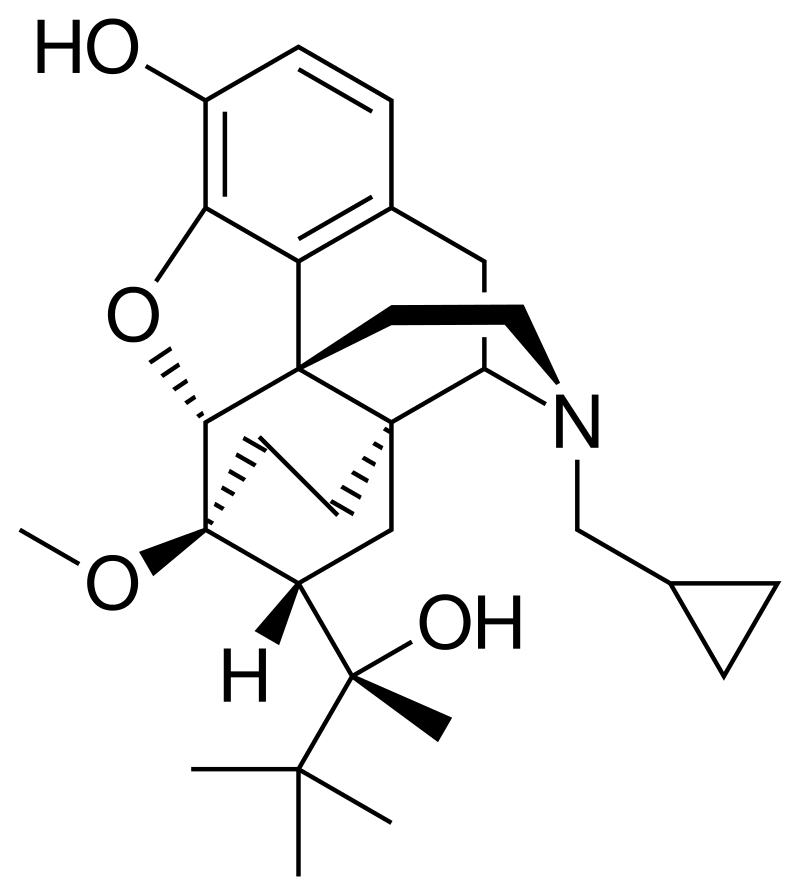
BUPRENORPHINE (Suboxone, Zubsolv, generics)
Buprenorphine is a medication that comes in film and tablet form. Buprenorphine decreases cravings and blocks the effects of all opioids. Patients on buprenorphine report feeling normal and welcome making positive choices the way they did prior to addiction. It is highly effective in achieving recovery. Patients on buprenorphine report feeling normal, functional and having a clear mind all day long, which allows them to make positive choices the way that they did prior to their addiction. When buprenorphine is combined with counseling and other forms of support, it can be highly effective in helping patients recover from addiction.

NALTREXONE (Vivitrol)
Naltrexone is a monthly injectable medication that decreases cravings and binds to receptors in the brain, preventing patients from feeling any pleasant effects from opioids or alcohol. Vivitrol may be initiated after opioid detoxification. It may also be used by patients who have completely tapered off of buprenorphine or methadone to prevent relapse.
Sublocade

IMPORTANT SAFETY INFORMATION FOR SUBLOCADE
IMPORTANT SAFETY INFORMATION
What is the most important information I should know about SUBLOCADE?
Because of the serious risk of potential harm or death from self-injecting SUBLOCADE into a vein (intravenously), it is only available through a restricted program called the SUBLOCADE REMS Program.
- SUBLOCADE is not available in retail pharmacies.
- Your SUBLOCADE injection will only be given to you by a certified healthcare provider.
INDICATION
SUBLOCADE™ (buprenorphine extended-release) injection, for subcutaneous use (CIII) is a prescription medicine used to treat adults with moderate to severe addiction (dependence) to opioid drugs (prescription or illegal) who have received an oral transmucosal (used under the tongue or inside the cheek) buprenorphine-containing medicine at a dose that controls withdrawal symptoms for at least 7 days. SUBLOCADE is part of a complete treatment plan that should include counseling.
In an emergency, you or your family should tell the emergency medical staff that you are physically dependent on an opioid and are being treated with SUBLOCADE.
Buprenorphine, the medicine in SUBLOCADE, can cause serious and life-threatening problems, especially if you take or use certain other medicines or drugs. Call your healthcare provider right away or get emergency help if you:
- feel faint or dizzy
- have mental changes such as confusion
- have slower breathing than you normally have
- have severe sleepiness
- have blurred vision
- have problems with coordination
- have slurred speech
- cannot think well or clearly
- have a high body temperature
- have slowed reflexes
- feel agitated
- have stiff muscles
- have trouble walking
These can be signs of an overdose or other serious problems.
Death or serious harm, including life-threatening breathing problems, can happen if you take anxiety medicines or benzodiazepines, sleeping pills, tranquilizers, muscle relaxants, or sedatives, antidepressants, or antihistamines, or drink alcohol during treatment with SUBLOCADE. Tell your healthcare provider if you are taking any of these medicines and if you drink alcohol.
SUBLOCADE is a controlled substance (CIII) because it contains buprenorphine that can be a target for people who abuse prescription medicines or street drugs.
Death has been reported in those who are not opioid dependent who received buprenorphine sublingually.
Do not use SUBLOCADE if you are allergic to buprenorphine or any ingredient in the prefilled syringe (ATRIGEL® Delivery System, a biodegradable 50:50 poly(DL-lactide-co-glycolide) polymer and a biocompatible solvent, N-methyl-2-pyrrolidone (NMP)).
SUBLOCADE may not be right for you. Before starting SUBLOCADE, tell your healthcare provider about all of your medical conditions, including:
- Trouble breathing or lung problems
- An enlarged prostate gland (men)
- A head injury or brain problem
- Problems urinating
- A curve in your spine that affects your breathing (scoliosis)
- Liver problems
- Gallbladder problems
- Adrenal gland problems
- Addison’s disease
- Low thyroid hormone levels (hypothyroidism)
- A history of alcoholism
- Mental problems such as hallucinations (seeing or hearing things that are not there).
- Are pregnant or plan to become pregnant. Opioid-dependent women on buprenorphine maintenance therapy may require additional analgesia during labor. If you receive SUBLOCADE while pregnant, your baby may have symptoms of opioid withdrawal at birth.
- Are breastfeeding or plan to breastfeed. SUBLOCADE can pass into your breast milk and may harm your baby. Talk with your healthcare provider about the best way to feed your baby during treatment with SUBLOCADE. Watch your baby for increased drowsiness and breathing problems.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins and herbal supplements. SUBLOCADE may affect the way other medicines work and other medicines may affect how SUBLOCADE works. Some medicines may cause serious or life-threatening medical problems when taken with SUBLOCADE. Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist each time you get a new medicine.
The doses of certain medicines may need to be changed if used during treatment with SUBLOCADE. Do not take any medicine during treatment with SUBLOCADE until you have talked with your healthcare provider. Your healthcare provider will tell you if it is safe to take other medicines during treatment with SUBLOCADE.
You should not take anxiety medicines or benzodiazepines (such as Valium® or Xanax®), sleeping pills, tranquilizers, muscle relaxants, or sedatives (such as Ambien®), antidepressants, or antihistamines that are not prescribed to you during treatment with SUBLOCADE, as this can lead to slowed breathing, drowsiness, delayed reaction time, loss of consciousness or even death. If a healthcare provider is considering prescribing such a medicine for you, remind the healthcare provider that you are being treated with SUBLOCADE.
You may have detectable levels of SUBLOCADE in your body for a long period after stopping treatment with SUBLOCADE.
What should I avoid while being treated with SUBLOCADE?
- Do not drive, operate heavy machinery, or perform any other dangerous activities until you know how this medicine affects you. Buprenorphine can cause drowsiness and slow reaction times. This may happen more often in the first few days after your injection and when your dose is changed.
- Do not drink alcohol during treatment with SUBLOCADE, as this can lead to slowed breathing, drowsiness, slow reaction time, loss of consciousness or even death.
What are the possible side effects of SUBLOCADE?
SUBLOCADE can cause serious side effects, including:
- Physical dependence and withdrawal. Your body can develop a physical need for SUBLOCADE (dependence). If you stop receiving SUBLOCADE, you could have opioid withdrawal symptoms such as:
- shaking, goose bumps, muscle aches
- sweating more than normal
- feeling hot or cold more than normal
- runny nose and watery eyes
- diarrhea or vomiting
These symptoms may start weeks to months after your last dose of SUBLOCADE.
- Liver problems. Call your healthcare provider right away if you notice any of these signs of liver problems:
- your skin or the white part of your eyes turns yellow (jaundice)
- urine turns dark
- bowel movements (stools) turn light in color
- decreased appetite
- stomach (abdomen) pain or nausea
Your healthcare provider may do tests before and during treatment with SUBLOCADE to check your liver.
- Allergic reaction. Call your healthcare provider or get emergency help right away if you get:
- rash, hives, itching
- swelling of your face
- wheezing
- dizziness, or a decrease in consciousness
- Decrease in blood pressure. You may feel dizzy when you get up from sitting or lying down.
- The most common side effects of SUBLOCADE include:
- constipation
- headache
- nausea
- injection site itching
- vomiting
- increase in liver enzymes
- tiredness
- injection site pain
- Long-term (chronic) use of opioids, including SUBLOCADE, may cause fertility problems in males and females. Talk to your healthcare provider if this is a concern for you.
These are not all the possible side effects. Call your healthcare provider for medical advice about side effects.
To report pregnancy or side effects associated with taking SUBLOCADE, please call 1-877-782-6966. You are encouraged to report negative side effects of drugs to the FDA. Visit www.fda.gov/medwatch or call 1-800-FDA-1088.
For more information about SUBLOCADE, see the full Prescribing Information including BOXED WARNING, and Medication Guide or talk to your healthcare provider. For REMS information visit www.sublocadeREMS.com.
You are encouraged to report negative side effects of drugs to the FDA. Visit www.fda.gov/medwatch or call 1-800-FDA-1088.
Find Additional Help with Supplemental Mental Health and Addiction Services
You may contact Connecticut State Department of Mental Health and Addiction Services. Find your local 24-Hour CRISIS Numbers
- Client Rights and Grievances
- Info Line (211) Connecticut Mental Health and Addiction Service Search
- SAMHSA Behavioral Health Treatment Services Locator
